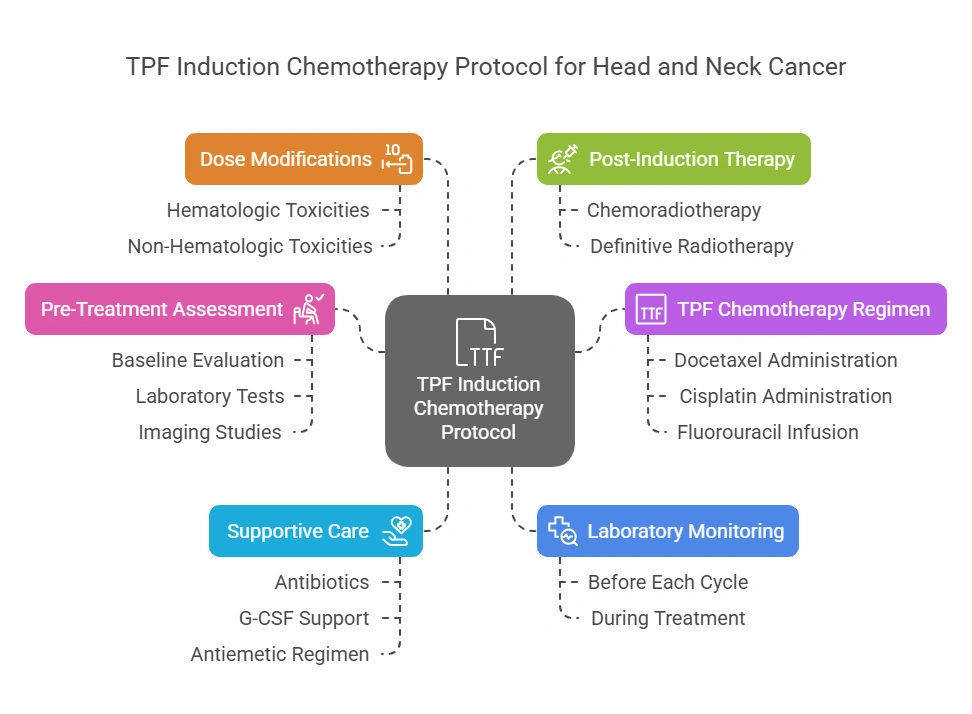
TPF Chemo Regimen
Based on the TAX 324 study published in NEJM, the following represents a comprehensive treatment protocol for TPF (docetaxel, cisplatin, fluorouracil) induction chemotherapy for locally advanced squamous cell carcinoma of the head and neck.
https://www.nejm.org/doi/full/10.1056/NEJMoa070956
Pre-Treatment Assessment Parameters
1. Baseline Evaluation:
- Complete history and physical examination
- Performance status assessment (WHO/ECOG ≤1 required)
- Baseline audiometry
- Nutritional assessment; consider prophylactic PEG placement
- Dental evaluation and necessary interventions
2. Laboratory Tests:
- Complete blood count with differential
- Comprehensive metabolic panel including:
- Renal function (creatinine clearance ≥60 mL/min)
- Liver function tests (AST, ALT, bilirubin ≤1.5× ULN)
- Electrolytes including magnesium, calcium, and phosphate
- Baseline albumin level
3. Imaging Studies:
- CT or MRI of head and neck
- CT of chest
- PET-CT (optional, for baseline staging)
TPF Chemotherapy Regimen
Repeat cycle every 21 days for 3 cycles:
1. Day 1:
- Docetaxel 75 mg/m² IV over 1 hour
- Followed by cisplatin 100 mg/m² IV over 1-3 hours
- Begin fluorouracil 1000 mg/m²/day as continuous IV infusion
2. Days 2-4:
- Continue fluorouracil 1000 mg/m²/day as continuous IV infusion (total 4-day infusion)
Pre-Medications
1. Docetaxel Pre-Medications (start 12-24 hours prior to docetaxel):
- Dexamethasone 8 mg PO BID for 3 days starting 1 day before chemotherapy
- Diphenhydramine 25-50 mg IV 30 minutes before docetaxel
- Ranitidine 50 mg IV (or equivalent H2 blocker) 30 minutes before docetaxel
2. Cisplatin Pre-Medications:
- Ondansetron 16 mg IV or palonosetron 0.25 mg IV day 1
- Dexamethasone 20 mg IV day 1 (can be integrated with docetaxel premedication)
- Aprepitant 125 mg PO day 1, followed by 80 mg PO days 2-3
- Olanzapine 5-10 mg PO day 1 (optional for high-risk patients)
IV Hydration Protocol
1. Pre-Cisplatin Hydration:
- Normal saline 1000-1500 mL with 20 mEq KCl and 2 g magnesium sulfate over 2-3 hours
2. Post-Cisplatin Hydration:
- Normal saline 1000-1500 mL with 20 mEq KCl and 2 g magnesium sulfate over 2-3 hours
- Continue IV hydration for 24-48 hours if outpatient administration not feasible
3. Mannitol Diuresis (optional):
- Mannitol 12.5-25 g IV before cisplatin
Supportive Care Medications
1. Prophylactic Antibiotics:
- Ciprofloxacin 500 mg PO BID (or levofloxacin 500 mg daily) starting day 5 of each cycle for 10 days
2. G-CSF Support (consider for high-risk patients):
- Pegfilgrastim 6 mg SC once on day 6, or
- Filgrastim 5 μg/kg SC daily starting day 5 until ANC recovery
3. Home Antiemetic Regimen:
- Days 1-4: Dexamethasone 8 mg PO BID (tapering schedule)
- Days 2-3: Aprepitant 80 mg PO daily
- Days 1-7: Ondansetron 8 mg PO Q8H PRN or 8 mg ODT Q12H PRN
- PRN: Prochlorperazine 10 mg PO/IV Q6H or metoclopramide 10-20 mg PO/IV Q6H
- PRN: Olanzapine 5-10 mg PO daily for breakthrough nausea
- PRN: Lorazepam 0.5-1 mg PO/IV Q6H for anticipatory nausea/anxiety
Laboratory Monitoring
1. Before Each Cycle:
- CBC with differential (ANC ≥1,500/μL, platelets ≥100,000/μL required)
- Comprehensive metabolic panel
- Magnesium, calcium, phosphate levels
- Creatinine clearance calculation
2. During Treatment:
- CBC weekly during cycles
- Electrolytes twice weekly when receiving cisplatin
- Liver function tests weekly for first cycle, then before each subsequent cycle
Dose Modifications
1. Hematologic Toxicities:
- Grade 4 neutropenia lasting >7 days: Reduce docetaxel to 60 mg/m²
- Febrile neutropenia: Reduce docetaxel to 60 mg/m²
- Grade 4 thrombocytopenia: Reduce cisplatin and fluorouracil by 25%
2. Non-Hematologic Toxicities:
- Grade 3-4 mucositis: Reduce fluorouracil by 25%
- Creatinine clearance 40-59 mL/min: Reduce cisplatin to 75 mg/m²
- Creatinine clearance <40 mL/min: Consider carboplatin substitution
- Grade 2 neuropathy: Reduce cisplatin by 25%
- Grade 3 neuropathy: Discontinue cisplatin
Post-Induction Therapy
As per the TAX 324 protocol, 3-8 weeks after the third cycle of induction chemotherapy, patients should proceed to:
- Chemoradiotherapy with weekly carboplatin (AUC 1.5)
- Definitive radiotherapy (70-74 Gy to primary tumor, 60-74 Gy to involved nodes, ≥50 Gy to uninvolved nodes)